Difference Between Vasculogenesis and Angiogenesis
A brief introduction to Vasculogenesis and Angiogenesis
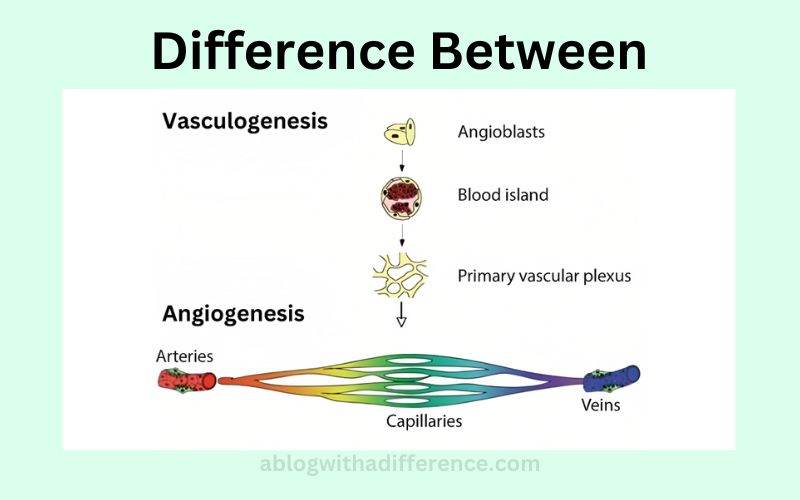
Angiogenesis and vasculogenesis differ significantly. Vasculogenesis refers to the formation of blood vessels during embryonic development. Angiogenesis refers to an increase in blood vessel formation during development.
Angiogenesis and vasculogenesis play an essential role in maintaining life. Angiogenesis is a natural process found throughout life that plays an essential role in Tissue repair. Angiogenesis also plays an essential part in cancer biology.
Importance of understanding the difference between vasculogenesis and angiogenesis
Understand the differences between angiogenesis and vasculogenesis is vitally important for numerous reasons:
1. Developmental Processes: Vasculogenesis plays a crucial role during embryonic development. Vasculogenesis involves the formation of new blood vessels by angioblasts, hematopoietic cells, and stem cells – contributing to an initial vascular system – while angiogenesis involves sprouting new vessels or remodeling old ones to form an established, functional system.
Understanding these processes is essential in understanding embryonic development as well as organogenesis processes.
2. Tissue Growth and Repair: Angiogenesis plays an essential part in tissue growth and repair. It provides oxygen, nutrients, and waste removal while simultaneously cleaning away waste products produced during growth.
Vasculogenesis on the other hand occurs during embryonic development; understanding their differences allows us to gain more insight into how blood vessels form tissues through processes like wound healing or tissue engineering.
3. Disease Pathology: Abnormal Angiogenesis has been linked with various pathologies including cancer, diabetic retinal disease, and Cardiovascular illnesses.
Researchers and clinicians will gain a more in-depth knowledge of these diseases if they understand the distinctions between vasculogenesis and angiogenesis, helping them create novel therapeutic interventions to control or modulate specific processes related to either one, thus controlling blood vessel formation in pathological scenarios.
4. Therapeutic Interventions: Therapeutic interventions may depend on distinguishing angiogenesis from vasculogenesis. Targeting vasculogenesis during embryonic development could have severe unintended side effects that lead to severe abnormalities.
Conversely, blocking pathological angiogenesis while sparing normal angiogenesis may provide safer and more effective solutions.
5. Research and Drug Development: Gaining insight into the differences between angiogenesis and vasculogenesis allows researchers to conduct more targeted experiments.
They can then use this knowledge to identify specific markers, pathways of signaling, and cell interactions involved with each process – information which will aid them in creating novel drugs or treatments to target either process to increase treatment outcomes and minimize potential side effects.
Understanding the difference between Vasculogenesis and Angiogenesis is crucial in comprehending vascular development tissue repair, and pathological processes as well as therapeutic interventions.
What Is Vasculogenesis?
Vasculogenesis refers to the formation of new blood vessels through spontaneous generation from precursor cells that eventually differentiate into endothelial cells and form functional blood vessels – often during embryonic development when circulatory systems begin taking shape.
Angioblasts are undifferentiated mesodermal cells that give rise to endothelial cells lining blood Vessels. Angioblasts, undifferentiated cells from the mesoderm, give rise to endothelial cell linings of these blood vessels while Hematopoietic cells contribute by differentiating into blood cells themselves and helping form a vascular network.
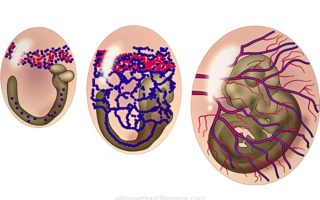
Vasculogenesis begins with the migration and accumulation of angioblasts, hematopoietic cells, and stem cells into specific regions of an embryo where new blood vessels will form.
After they accumulate there, precursor cells differentiate into endothelial cells which then align and organize themselves to form primitive vascular structures known as blood islands; within them, endothelial lining cells form hollow tubes which eventually fuse together to form primary blood vessels.
Vasculogenesis can be controlled through various signaling pathways and growth factors, with VEGF being an influential player. Notch and Wnt signaling pathways also play key roles in vasculogenesis by helping mature blood vessels into patterns.
Vasculogenesis, which typically occurs during embryonic development, establishes the initial blood vessel network. Angiogenesis then provides further blood vessel growth and remodeling after this initial stage has passed – this may involve sprouting new vessels or expanding existing ones.
Understanding the mechanisms and regulators underlying vasculogenesis is central to embryonic development and unraveling any complex vascular disorders or developments that occur during this stage.
What Is Angiogenesis?
Angiogenesis refers to the process of producing new blood vessels by creating connections among existing ones it does not refer to creating entirely new blood vessels from scratch.
Angiogenesis occurs throughout life. Angiogenesis is an ongoing process while vasculogenesis typically only appears during early development. Angiogenesis plays a vital role in repairing damaged blood cells.
Angiogenesis occurs when damaged or injured cells begin to sprout new blood vessels. Endothelial cells then secrete metalloproteases which digest the basement membrane, and eventually escape into peripheral tissues where they will lead to cell proliferation in new locations.
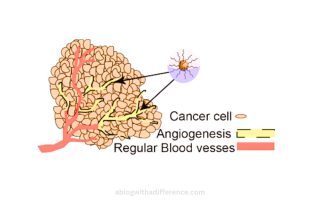
Angiogenesis increases during cancer. Angiogenesis accelerates because expression of the Vascular Endothelial Growth Factor (VEGF) increases, providing more nutrients to cancerous cells that proliferate, thus increasing cell stability.
Differences between Vasculogenesis and Angiogenesis
Vasculogenesis differs significantly from angiogenesis in several key ways:
1. Origin of Blood Vessel Formation:
- Vasculogenesis: Vasculogenesis refers to the creation of new blood vessels by angioblasts or Hematopoietic cells. Blood vessels arise from precursor cells that did not previously exist.
- Angiogenesis: Angiogenesis refers to the formation and remodeling of new blood vessels through endothelial cell proliferation and migration; existing vessels sprout new blood vessels as preexisting ones expand or rupture to give way.
2. Timing and occurrence:
- Vasculogenesis: Vasculogenesis occurs mainly during embryonic development when the circulatory system is established.
- Angiogenesis: Angiogenesis is a process that occurs under various Physiological and pathological circumstances such as tissue growth, wound healing, or illness such as cancer.
3. Cell Types Involved:
- Vasculogenesis: Vasculogenesis is a process in which blood vessels are formed through the combined activity of hematopoietic cells and angioblasts, mesodermal stem cells which have not yet been Differentiated into mature vessels.
- Angiogenesis: Angiogenesis is a process primarily driven by endothelial and supporting cells; specifically pericytes and endothelial cells form the inner linings of blood vessels during this process.
4. Regulation and Signal Pathways:
- Vasculogenesis: Vasculogenesis, which can be controlled via different signaling pathways such as vascular endothelial growth factor (VEGF), Wnt signaling, and Notch signaling, involves many cells producing new blood vessels to Accommodate new organs or parts of existing ones.
- Angiogenesis: Angiogenesis can also be controlled via signaling pathways such as VEGF. Additionally growth factors like FGFs and PDGFs play an essential role in Angiogenesis.
Although angiogenesis and vasculogenesis differ significantly, both processes are interlinked and may impact one another.
Angiogenesis, on the other hand, involves further blood vessel growth and remodeling as a response to physiological or pathological Circumstances both processes play an integral part in tissue repair and maintenance.
Mechanisms of Vasculogenesis and Angiogenesis
Vasculogenesis and angiogenesis occur due to an intricate series of cellular and molecular processes that occur simultaneously.
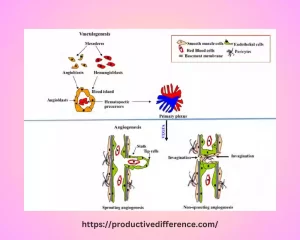
So here is an overview of key mechanisms involved:
Vasculogenesis:
1. Angioblast Differentiation: Vasculogenesis begins with the differentiation of angioblasts – precursor cells from mesodermal and hemangioblastic lines which become committed to endothelial lineages after maturing through differentiation.
2. Vascular Guidance and Coalescence: Angioblasts migrate to specific sites where they form blood islands – clusters of angioblasts surrounded by basement membranes. Over time, the blood islands coalesce into primitive vascular plexus which later develops into primary vascular networks.
3. Lumen Formation: Endothelial cells in primitive vascular systems undergo lumen formation when connecting, creating an empty and fluid-filled cavity called the lumen. This humanization allows blood vessels to form and function effectively.
Angiogenesis:
1. Endothelial Activation: Angiogenesis can be stimulated by hypoxia or inflammation signals, activating quiescent endothelial cells present in existing blood vessels into becoming active and initiating the angiogenic processes.
2. Degradation of Basement Membranes: Endothelial cell activation releases matrix metalloproteinases which degrade the basement membrane surrounding cells, enabling them to migrate and breach through.
3. Endothelial Cell Migration: Active endothelial migratory cells migrate towards an angiogenic stimulant or growth factor gradient by extending lamellipodia and filopodia to allow cell movement within tissue.
4. Endothelial Cell Proliferation: Proliferation of endothelial migratory cells leads to solid sprouts with tip cells in front and stalk cells behind. Chemotactic signals control how many tip cells will grow into these solid sprouts.
5. Tube Formation and Anastomosis: At the leading edge of a tube, cells form connections with endothelial cells to form a hollow tube. Stalk cells provide support to sprouts that branch out and elongate. Anastomosis allows further connections to be made between sprouts and existing vessels through anastomosis to create functional vessels.
6. Vessel Stabilization and Maturation: Newly formed blood vessels require maturation as part of their evolution into functional networks of blood vessels. Pericytes, smooth muscle cells, and other cell types are recruited onto vessel walls in order to provide structural support and promote vessel stability, with pericytes providing extra reinforcement by providing structural support through recruitment on vessel walls and recruiting other cell types as needed for stabilization purposes.
Remodeling takes place to bring this vision of maturity closer.
These mechanisms involve an intricate interplay of signaling molecules and growth factors with extracellular matrix components, cell adhesion molecules and cell interactions to ensure blood vessels form, remodel and function properly in vasculogenesis and angiogenesis processes.
Understanding these mechanisms will allow us to develop therapeutic strategies for modulating Angiogenesis and Vasculogenesis in different contexts such as tissue engineering or wound healing.
Factors Influencing Vasculogenesis and Angiogenesis
Vasculogenesis or angiogenesis can be affected by multiple factors both intrinsic and extrinsic to it; these control the formation, growth, and remodeling of blood vessels.
They’re the main ones responsible for vasculogenesis or angiogenesis:
1. Growth Factors: Growth Factors are instrumental to vasculogenesis, angiogenesis and vascular development by stimulating proliferation, migration and differentiation of endothelial cells.
One such growth factor involved in angiogenesis is Vascular Endothelial Growth Factor (VEGF), an important survival and maintenance signal which triggers new blood vessel formation. Other growth factors also play roles such as FGFs (fibroblast-derived growth factors) PDGF (platelet-derived growth factor) or angiopoetins
2. Extracellular Matrix: The extracellular matrix surrounds cells to provide structural support, but its main influence on angiogenesis and vasculogenesis lies elsewhere: as an essential scaffold guiding blood vessel formation while aiding endothelial migration.
ECM components collagen, laminin, and fibronectin interact directly with endothelial cells during vessel development to increase adhesion, proliferation, and migration processes.
3. Oxygen and Hypoxia: Oxygen plays an essential part in vasculogenesis; low oxygen levels or hypoxia act as an effective stimulant of angiogenesis, activating hypoxia-inducible factor transcription factor HIF that controls pro-angiogenic factor VEGF expression to create new vessels which bring vital oxygen and nutrition directly to hypoxic tissue. This response results in new blood vessel growth providing a fresh supply of hypoxia tissues.
4. Inflammatory signals: Inflammation is caused by immune cell recruitment the release of Proinflammatory cytokines and chemokines, and other cytokines. This produces Proangiogenic signal such as TNF-a, (tumor-necrosis factor-alpha), as well as the interleukins IL-1, and IL-8, which stimulates angiogenesis via endothelial migration and proliferation. These can also promote tumor necrosis-factor-alpha, which activates
5. Extracellular Matrix Interactions: Extracellular matrix interactions play a crucial role in angiogenesis and vasculogenesis. Adherence molecules such as cadherins and integrins allow cell-to-cell contact as they promote endothelial migration during blood vessel growth and new vessel formation, and these relationships allow endothelial cells to coordinate movements during vessel formation processes.
6. Mechanical Forces: Mechanical forces such as tensional or shear forces may influence vasculogenesis, while shear stress caused by blood flow can impact endothelial cell behavior such as migration, proliferation, and alignment. Mechanical forces can modulate gene expression pathways involved with vessel remodeling or formation as well as remodeling/formation itself.
7. Genetic and Epigenetic Effects: Genetic factors and epigenetic modifications such as DNA methylation or histone modifications can Significantly impact vasculogenesis. Mutations or variations to genes involved with vessel development may lead to abnormalities that impair vasculogenesis; while epigenetic modifications like DNA methylation or histone modification can alter gene expression patterns affecting angiogenesis/vasculogenesis processes.
Understanding how these factors interact to impact vasculogenesis and angiogenesis processes under both physiological and pathological circumstances is integral for developing strategies to regulate these processes. Researchers aim to manipulate these factors so as to promote tissue regeneration and efficient blood vessel formation; also seeking new therapeutic approaches against diseases related to aberrant vascular remodeling or growth.
Comparison Chart of Vasculogenesis and Angiogenesis
Here is a chart that highlights the main differences between angiogenesis and vasculogenesis:
| Topics | Vasculogenesis | Angiogenesis |
|---|---|---|
| Definition | Formation of new blood vessel de novo in embryonic development | The sprouting of new blood vessels and the remodeling of existing vessels |
| A Occurrence | Primarily in embryonic development | In various physiological and pathological situations throughout life |
| Cell Types involved | Angioblasts, hematopoietic cells and stem cells | Endothelial and pericytes |
| Source of Blood Vessels | De novo formation | Spouting from existing vessels |
| Timing | Early stages of embryonic Development | Diseases, tissue growth, and wound healing |
| The Regulations of the United States | Signaling pathways for VEGF Notch and Wnt | Signaling pathways for VEGF FGF and PDGF |
| Purpose | The initial vascular network is established | Expands and remodels the blood vessels to promote tissue growth and repair |
| Significance | Essential for embryonic development | The role of fibroblasts in disease progression and tissue regeneration |
| Targeted Therapies | Not usually targeted therapeutically | The treatment of disease can target either the inhibition or promotion angiogenesis. |
Similarities between Vasculogenesis and Angiogenesis
There are both similarities and distinctions between angiogenesis and vasculogenesis:
1. Blood vessel formation: Vasculogenesis and angiogenesis both play key roles in blood vessel formation. Angiogenesis (also referred to as vasculogenesis) plays a pivotal role in blood vessel growth under different Circumstances.
2. Involvement of growth factors: Growth factors play an integral part in both processes. One such growth factor, called Vascular Endothelial Growth Factor or VEGF, serves as a key regulator of both angiogenesis and vasculogenesis by stimulating endothelial cell proliferation migration, and survival aiding blood vessel formation in turn.
3. Importance for tissue development and repair: Vasculogenesis is crucial for tissue development and repair. Angiogenesis and vasculogenesis play key roles in tissue formation and repair, providing essential tools for tissue improvement and regeneration.
4. Contributions to Homeostasis: Both processes contribute towards maintaining vascular homeostasis. For tissue perfusion, oxygenation, and nutrient delivery in different physiological contexts to be maintained, blood vessels must form and remodel themselves appropriately.
5. Signaling Pathways That Intersect: Though each process follows different pathways, many of those which regulate vasculogenesis and angiogenesis share common signals and pathways; one such signaling pathway that regulates both processes – in this instance VEGF which stimulates endothelial proliferation and migration- also overlap.
6. Clinical relevance: Vasculogenesis and Angiogenesis both play important roles in clinical medicine. An understanding of their processes may have implications for managing diseases, therapeutic interventions, and drug development in various pathologies such as cancer or cardiovascular disease; targeting specific aspects of angiogenesis or vasculogenesis could potentially offer treatments.
Vasculogenesis differs from angiogenesis in several key respects, yet both processes share many similarities, such as their roles in blood vessel formation, involvement of growth factors, the contribution of tissue repair and development, and the effect on homeostasis.
Both also possess interlocking signaling paths as well as clinical relevance – understanding each process is vital for understanding blood vessel formation as well as related physiological or pathological conditions.
Conclusion
Understanding the differences between vasculogenesis and angiogenesis is critical to understanding blood vessel Biology and its roles in various Physiological and pathological conditions. Angiogenesis refers to the development of new vessels or remodeling of existing ones that play an essential part in growth healing, or disease processes.
Understanding these processes will enable researchers and clinicians to gain a better grasp of their mechanisms, leading to advances in developmental biology and tissue engineering. Furthermore, this will identify key signaling pathways and growth factors involved in blood vessel development.