14 Things Only Die-Hard Fans Get About L-form Bacteria and Mycoplasma
A Brief Overview of L-form Bacteria and Mycoplasma
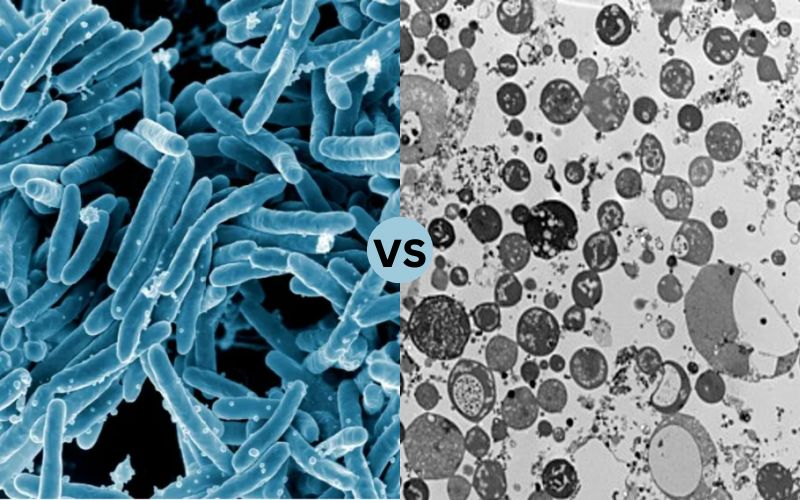
L-form bacteria and Mycoplasma share the characteristic absence of an intact cell wall, leading them to form unique shapes with irregular edges, show greater antibiotic resistance and have more medical relevance than their conventional cell-walled counterparts.
L-form bacteria are non-traditional variants that lack rigid cell walls, adapting to various shapes to form infections more effectively and resist antibiotic treatment. L-forms can form under stress conditions from normal bacteria, potentially leading to persistent infections and antibiotic resistance. Mycoplasma are self-replicating organisms without cell walls but possess unique cell membrane composition.
Mycoplasma species play roles in human and animal diseases most notably Mycoplasma pneumoniae which causes respiratory infections. Both L-forms and Mycoplasma present challenges to conventional microbiology due to their unique characteristics and medical implications requiring research efforts in order to understand them fully as well as develop effective diagnostic and treatment strategies.
What are L-form Bacteria
L-form, also known as “L-phase” bacteria are bacteria without cells with walls. They are derived from several bacteria. The L-form bacteria could possibly revert to their initial or parent in certain conditions. The absence of the cell wall is not an inherent feature of the L-form bacteria. The cells have formed with no cell walls because due to a mutation, or due to nutritional stress.
The year 1935 was the time that Emmy Klieneberger Nobel found L-form bacteria at first. L-form bacteria resemble mycoplasma. In contrast to mycoplasma, L-form bacteria are not normal bacteria. The L-form bacteria can be sensitive to the osmotic stress. Furthermore, the L-form bacterium is susceptible to osmotic shock. Gram-positive or gram-negative. They come in a variety of forms.
What is Mycoplasma?
Mycoplasma is a family of bacteria which lacks the cell wall that surrounds their membranes. They are among the tiniest and the simplest of bacteria. They are the only bacteria with a minimal amount of organelles in their cells.
They fall under the category of Mollicutes. Mycoplasma is mostly spherical form. Mycoplasma causes diseases for both animals and human beings. Since mycoplasma is not able to form an internal cell wall, it can’t be treated with antibiotics that target cells.
They are able to be destroyed through the use of extremely either low or high salt environments. They cannot withstand the surrounding osmotic conditions. The steroid-rich membrane helps to prevent them from rupturing.
Mycoplasma-related infections are among the most significant issues within cell culture and research labs. In addition, mycoplasma is controlled with certain antibiotics, like macrolides, tetracyclines, and the more recent quinolones to which they are highly sensitive.
History of L-form Bacteria and Mycoplasma
History of L-form Bacteria:
Discovering L-form bacteria dates back to the 1930s when researchers Frederick Griffith and J.B.S Haldane first observed unusual cell wall-deficient forms while investigating Streptococcus pneumoniae. Emmy Klieneberger-Nobel coined the term “L-form” after witnessing abnormal forms that lacked cell walls that she identified.
In the 1960s and 70s, researchers like Jean-Pierre Jeljaszewicz and Miroslav Radman investigated L-form bacteria more closely, studying their formation and implications. These researchers discovered that L-forms could arise from various species under stress conditions.
Their shapes showed pleomorphism; which increased antibiotic resistance. Their investigation led them further as researchers explored their role in chronic infections, and biofilm formation, as experimental tools in genetic studies or even their potential as experimental tools themselves.
Histories of Mycoplasma: The history of Mycoplasma dates back to the early 20th century when researchers like Albert J. Mycoplasma, and Edward Klieneberger identified an organism smaller and simpler than typical bacteria. But only in 1950 did researchers realize these organisms did not possess cell walls separating them from other types.
Edward Klieneberger-Nobel first suggested Mycoplasma in 1962 to describe wallless microorganisms such as Mycoplasma pneumoniae as being responsible for human “walking pneumonia” cases during his early 1960s study of Mycoplasma infections. Since this discovery of its pathogenic potential has only become clear since.
Mycoplasma species have been implicated in multiple human, animal, and plant illnesses. Research efforts have centered around understanding their unique biology, genetics, and pathogenic mechanisms, as well as advancements in molecular techniques that enable better diagnostics while offering insights into the diversity and evolution of Mycoplasma species.
Understanding the Unique Characteristics of L-form Bacteria and Mycoplasma
Understanding the Unique Properties of L-form Bacteria and Mycoplasma:
L-form Bacteria:
- Cell Wall Absence: L-form Bacteria are distinguished from typical bacteria by the lack of conventional cell walls that characterise most strains, as well as by their unique ability to adopt multiple shapes and sizes – unlike typical strains which only possess fixed forms.
- Pleomorphic Shape: They exhibit what’s known as pleomorphism – meaning their shapes change without clear definition from bacteria with fixed forms.
- Stress-Induced Formation: L-forms may appear when normal bacteria come under stress from antibiotics or other factors that alter their environments, including antibiotic usage or harsh environments.
- Antibiotic Resistance: Due to lacking cell wall targets, L-forms often exhibit increased resistance to antibiotics that target cell wall synthesis.
- Genetic Instability: L-forms have also been known to display genomic instability or aneuploidy leading to further diversity within their characteristics.
- Implications in Infections: L-forms have long been implicated as contributing to persistent infections that contribute to chronicity of certain diseases.
- Medical Relevance: medical relevance including implications for antibiotic resistance mechanisms and treatment strategies (Mycoplasma in particular).
Mycoplasma:
- Cell Wall Absence: Mycoplasma stands out from most bacteria by lacking conventional cell walls, giving rise to greater diversity through pleomorphism and allowing pleomorphism.
- Unique Cell Membrane: They possess an unique cell membrane rich with sterols which contributes to structural integrity, further distinguishing themselves.
- Reduced Genome Size: Mycoplasma species possess small genomes with few genes, placing a heavy dependence on host environments for nutrients.
- Pathogenic Diversity: Their pathogenic variety impacts humans, animals, and plants alike – further underscoring their medical and ecological importance.
- Culturing: Mycoplasmas can be difficult to cultivate due to their fastidious nature, necessitating special growing conditions for them to flourish in. Diagnostic
- Techniques: Given their peculiar traits and cultivation difficulties, molecular techniques often become the go-to way of detection when looking for Mycoplasma infections.
- Host Sensitivity: Certain Mycoplasma species exhibit host specificity, leading to specific diseases in particular hosts.
- Biotechnological Potential: Due to Mycoplasma’s small genome size and thus biopharmaceutical production potential.
- Research Importance: Investigating Mycoplasma can give researchers insight into its pathogenic mechanisms, host interactions and possible therapeutic targets.
key differences between L-form bacteria and Mycoplasma
Here’s a comparison chart highlighting the key differences between L-form bacteria and Mycoplasma:
| Aspect | L-form Bacteria | Mycoplasma |
|---|---|---|
| Cell Wall | Absent | Absent |
| Formation | Stress-induced, loss of cell wall | Evolutionary loss of cell wall |
| Shape | Pleomorphic | Pleomorphic |
| Genetic Complexity | Genomic instability, potential aneuploidy | Simple genomes, reduced metabolic capabilities |
| Size | Variable | Generally small |
| Gram Staining | Variable | N/A (due to lack of cell wall) |
| Reproduction | Binary fission | Binary fission |
| Antibiotic Resistance | Increased resistance due to lack of target (cell wall) | Varies among species |
| Medical Significance | Implicated in chronic infections, antibiotic resistance | Cause of various human, animal, and plant diseases |
| Host Specificity | Not as clearly defined | Some species specific to certain hosts |
| Culturing Difficulty | Requires special conditions | Challenging due to fastidious nature |
| Diagnostic Techniques | Microscopy, molecular techniques | Molecular methods, specialized culture |
| Research Focus | Pleomorphism, antibiotic resistance | Pathogenicity, host interactions, diagnostics |
| Biotechnological Uses | Potential in genetic engineering | Biopharmaceutical production |
What are the Similarities Between L-form Bacteria and Mycoplasma?
Mycoplasma and L-form bacteria share an uncanny similarity when it comes to structural adaptations: both lack an outer cell wall. This set apart these organisms from typical bacteria and influences various aspects of their biology.
- Cell Wall Deficiency: L-form bacteria and Mycoplasma both lack rigid peptidoglycan cell walls found in most bacteria, providing their unique characteristics. This represents a fundamental departure from structural norms, leading to their unique features.
- Pleomorphic Shapes: Since their cells lack rigid walls, both L-form bacteria and Mycoplasma exhibit pleomorphism – the ability to assume various shapes and sizes due to structural abnormalities – an effect directly linked to their shared structural anomaly.
- Problems in Antibiotic Susceptibility: Beta-lactam antibiotics that target cell wall synthesis, like beta-lactams, tend to be ineffective against both L-form bacteria and Mycoplasma due to a lack of target sites impede their efficacy, leading to parallel resistance mechanisms.
- Medical Implications: Although each type is structurally distinct, both have medical applications. L-form bacteria have been linked with chronic infections and antibiotic resistance while Mycoplasma species have caused diseases in different hosts indicating their shared significance as diseases spread among hosts.
- Adaptation to Stress: Both L-form bacteria and Mycoplasma lack cell walls, making them susceptible to environmental stressors such as environmental osmotic changes and other environmental stresses, leading to their own unique strategies of adaptation and survival. This vulnerability shapes their evolutionary adaptations over time.
How are L-form bacteria and Mycoplasma treated?
Treatment plans for L-form bacteria and Mycoplasma vary based on each species’ unique traits and challenges;.
Here is an overview:
L-form Bacteria:
L-form bacteria present unique challenges because of their adaptability and antibiotic resistance, since they do not produce conventional cell walls like beta-lactams do, rendering these medications often ineffective against them.
Potential treatments could include:
- Combination Therapy: Antibiotics with various mechanisms of action may be combined in order to address multiple vulnerabilities present in L-forms. Non-
- Traditional Antibiotics: Alternative antibiotics which target other cell processes or targets should also be considered.
- Stress Management: Preventing or minimizing stressful transitions towards L-forms might help limit their emergence.
- Immunotherapy: Strengthening immune response could aid in clearing infections caused by L-forms.
Mycoplasma:
Mycoplasma infections must be approached individually according to both species involved and host condition, with antimicrobial susceptibility varying depending on which variety infected; treatment options might include antibiotics.
- Antibiotics: Antibiotics for Mycoplasma infections include macrolides, tetracyclines and fluoroquinolones – each will depend on which species and its resistance pattern are being targeted.
- Culture-Directed Therapy: Acknowledging the exact Mycoplasma species through culture and susceptibility testing helps tailor antibiotic treatment.
- Adjunct Therapies: Supplementing supportive care by managing symptoms may aid recovery in cases with more serious infections.
- Antibiotic Stewardship: Due to growing antibiotic resistance, prudent usage of antibiotics is crucial in order to forestall further resistance development in resistant strains.
Prevention Techniques for Mycoplasma and L-form Bacterial Infections
Preventing L-form bacteria and Mycoplasma infections requires taking an integrated approach in order to limit exposure, transmission, and complications. Antibiotic use should always be managed appropriately as certain antibiotics may contribute to L-form conversion in healthcare settings, good hygiene and infection control measures, especially among healthcare staff are particularly essential to help stop their spread among individuals.
Understanding any triggers that contribute to L-form development such as stress or antibiotic exposure can reduce risks significantly – helping keep L-form infections under control in an effort to lower infection rates.
Preventing Mycoplasma infections involves both behavioral changes and healthcare practices. Engaging in safer sexual behaviors and adopting animal handling safety procedures are just two effective measures that can lower the risk of Mycoplasma transmission.
Implementing biosecurity measures in agricultural settings is vital in protecting livestock and crops against Mycoplasma infections, and helping stop its spread among livestock and crops.
Appropriate diagnosis and therapy with antibiotics are critical in controlling Mycoplasma infections and halting their progression into severe disease. Additionally, raising public awareness and education about transmission methods and early detection is crucial in order to equip individuals to take preventive steps themselves.
A comprehensive approach that includes hygiene practices such as responsible antibiotic usage and biosecurity protocols as well as informed healthcare decisions is required in order to avoid L-form bacteria or Mycoplasma infections altogether.
Summary
Prevention of L-form bacteria and Mycoplasma infections requires taking an approachable, comprehensive approach. With respect to L-form bacteria infections, such as those caused by antibiotics overuse or poor hygiene can mitigate risks while understanding stress triggers can also play a crucial role.
When it comes to Mycoplasma infections however, safe practices within human interactions and agriculture settings as well as timely diagnosis with antibiotic therapy treatment is paramount in their prevention.
public awareness campaigns play key roles as public awareness helps educate on responsible behavior choices which reduce stressors while informing healthcare decisions can help significantly limit their spread and impact preventing outbreaks from L-form bacteria and Mycoplasma infections from spreading or having adverse impact.