15 Brutal Truths About the Difference Between DKA and HHS
Overview of DKA and HHS
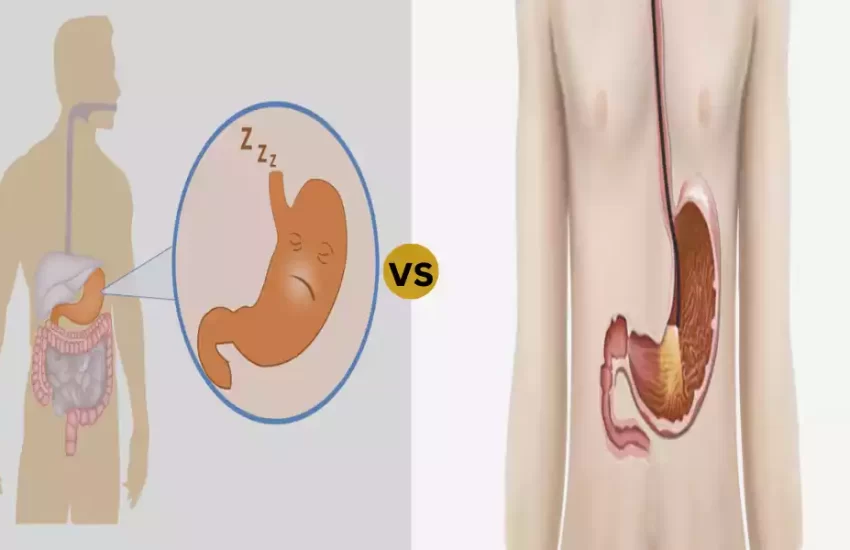
DKA and HHS are two serious complications of diabetes mellitus. DKA occurs due to an insufficient supply of insulin resulting in elevated blood sugar levels that stimulate the production of ketones, leading to metabolic abnormalities. Acidity causes an acidic environment with symptoms including excessive thirst, nausea, and rapid breathing.
Meanwhile, High Blood Sugar Syndrome (HHS) is marked by extremely high blood sugar levels without significant ketone production. HHS results from relative insulin deficiency combined with severe dehydration caused by osmotic diuresis.
Neurological symptoms like confusion and visual disturbances tend to be more prominent with HHS than DKA; each condition has unique diagnostic criteria, management approaches and potential complications; prompt recognition and treatment are therefore vitally important in both cases to avoid potentially life-threatening results.
What is Diabetic Ketoacidosis (DKA)
Diabetic Ketoacidosis (DKA) is a serious complication often seen among those living with type 1 diabetes but may also occur in those living with type 2. It arises due to a severe deficiency of insulin which prevents cells from using glucose for energy, leading to fat breakdown for energy production instead. An accumulation of ketones in the blood leads to acidosis or an acidic condition.
DKA (diabetic ketoacidosis) is characterized by elevated blood glucose levels (hyperglycemia), elevated ketone levels and metabolic acidosis. Symptoms typically develop rapidly, including excessive thirst, frequent urination, abdominal pain, nausea and vomiting as well as rapid and deep breathing (Kussmaul breathing) along with rapid or deep breathing that leads to Kussmaul breathing accompanied by fruity or acetone-like breath odor.
DKA requires immediate medical intervention. Treatment typically entails administering insulin to lower blood glucose levels and stop ketone production, as well as fluid replacement to counter dehydration caused by excessive urine production.
Electrolyte imbalances, particularly potassium levels, must also be carefully managed while monitoring blood glucose, ketone levels, electrolytes, and acid-base balance guides the treatment process.
DKA can result in serious complications, including cerebral edema, electrolyte imbalances, and even death if left untreated. For people living with diabetes to avoid DKA altogether, education about early signs, regular glucose monitoring, and proper insulin management as well as seeking medical help when hyperglycemic episodes arise are vital parts of preventative healthcare measures to keep blood sugar stable.
Characteristics of DKA
Diabetic Ketoacidosis (DKA) is an often fatal complication of diabetes, particularly type 1. However, it can also occur with type 2 diabetes and has several key
characteristics including:
- Hyperglycemia: Blood glucose levels become significantly elevated, typically surpassing 250 mg/dL (13.9 mmol/L).
- Ketosis: When insulin levels drop too low, our bodies start breaking down fat for energy production instead, producing ketones which build up in our blood and urine and cause metabolic acidosis causing metabolic acidosis and metabolic acidosis respectively.
- Metabolic Acidosis: Ketone buildup creates an acidic environment, decreasing blood pH levels and upsetting your body’s acid-base balance.
- Symptoms: People living with DKA may experience excessive thirst (polydipsia), frequent urination (polyuria), intense hunger (polyphagia), nausea, vomiting, abdominal pain and general malaise.
- Kussmaul Breathing: Rapid, deep and labored breathing known as Kussmaul breathing is an adaptive mechanism used by your body to eliminate excess acids through your lungs.
- Fruity Breath Odor: Acetone, one of the ketones, can produce an unpleasant fruity or nail polish-like odor in the breath, often due to an accumulation.
- Dehydration: Due to excessive urination and fluid loss, severe dehydration may develop, leading to dry skin, dry mouth, sunken eyes and reduced skin turgor.
- Electrolyte Imbalance: Potassium levels may initially increase as a result of acidosis; however, once insulin therapy begins to work they often drop quickly posing a risk for cardiac arrhythmias.
- Mental Status Changes: As DKA progresses, individuals may become increasingly lethargic and confused, potentially progressing into unconsciousness.
- Precipitating Factors: Diabetic Ketoacidosis can be caused by infections, missed insulin doses, illness, stress or undiagnosed diabetes.
- Lab Results: Diagnostic criteria for DKA typically include blood glucose levels above 250 mg/dL (13.9 mmol/L), arterial pH below 7.3, bicarbonate concentration below 18mEq/L, and the presence of ketones in blood or urine samples.
What are the causes of DKA?
Diabetic Ketoacidosis (DKA) occurs due to an unexpected shortage of insulin; typically seen among individuals living with type 1 diabetes, but potentially also possible under certain circumstances for individuals living with type 2 diabetes. DKA is caused by inadequate insulin levels, often as the result of missed injections, newly diagnosed cases of diabetes, pump malfunctions or insufficient dosage.
Sicknesses, infections and physical or emotional stress can elevate blood glucose levels by increasing demand for insulin or producing stress hormones that inhibit its effectiveness.
Corticosteroid use, certain medical conditions like pancreatitis and pregnancy in women with diabetes, substance abuse and abrupt changes in diabetes medication can all play a part in Diabetic Ketoacidosis (DKA) development. Therefore, understanding its triggers is imperative for individuals living with diabetes so as to effectively manage their condition and avoid life-threatening complications.
Symptoms of DKA
Diabetic Ketoacidosis (DKA) often manifests rapidly and its symptoms include:
- Excessive Thirst (Polydipsia): Individuals may experience extreme thirst and consume large volumes of water to quench it.
- Frequent Urination (Polyuria): High blood glucose levels lead to more frequent urination.
- Extreme Hunger (Polyphagia): Cells become depleted of glucose, leading to persistent feelings of hunger.
- Nausea and Vomiting: Nausea, vomiting and abdominal pain are the three primary symptoms.
- Rapid Breathing (Kussmaul Breathing): As the body tries to rid itself of excess acids via its lungs, breathing becomes deep and rapid in order to expel any acid waste through the system.
- Fruity Breath Odor: Due to acetone and other ketones present, your breath may have an acetone-like fruity or floral odor.
- Fatigue and Weakness: Low glucose production may result in fatigue and weakness throughout your body, contributing to overall fatigue and weakness.
- Confusion or Alterations to Mental Status: As DKA worsens, symptoms like confusion, difficulty focusing and even loss of consciousness may arise.
- Dehydration symptoms: Dry mouth, skin dryness, sunken eyes and decreased skin turgor due to severe fluid loss are some telltale signs.
- Rapid Heart Rate and Low Blood Pressure: Dehydration and electrolyte imbalance can result in rapid heart rate and low blood pressure, often simultaneously.
What is Hyperosmolar Hyperglycemic State (HHS)
Hyperosmolar Hyperglycemic State, more commonly referred to as Hyperosmolar Hyperglycemic Nonketotic Syndrome (HHNS), is a serious diabetic complication most often seen among older individuals or those with impaired kidney function with type 2 diabetes. HHS typically progresses more gradually than diabetic ketoacidosis (DKA) and manifests as extremely high blood glucose levels of 600 mg/dL or above.
HHS results from a relative deficiency of insulin, preventing cells from using glucose for energy and leading to excessive glucose buildup in the bloodstream and leading to symptoms like diuresis, dehydration, and electrolyte imbalances. Unlike DKA however, this condition does not involve significant ketone production or acidosis; yet blood becomes highly concentrated with glucose.
HHS symptoms include extreme thirst, frequent urination, confusion, altered consciousness, visual disturbances, and weakness – symptoms which if untreated can progress to seizures, coma, and even death.
Emergency medical attention for HHS is absolutely essential, with intravenous fluids provided intravenously to rehydrate and correct electrolyte imbalances, gradually decreasing blood glucose levels using insulin therapy, as well as identifying any contributing triggers like infections or medications that could have contributed to it.
Preventing HHS involves carefully monitoring blood glucose levels, taking all prescribed medications as directed, and seeking medical assistance if symptoms of hyperglycemia arise.
Individuals at risk must educate themselves on diabetes management, maintaining adequate hydration levels and recognizing any signs of declining health to mitigate HHS risks.
Characteristics of HHS
Hyperosmolar Hyperglycemic State, more commonly referred to as hyperosmolar Hyperglycemic Nonketotic Syndrome (HHNS), is a severe diabetic complication most often observed among individuals living with type 2 diabetes.
Its characteristics include:
- Extreme Hyperglycemia: Blood glucose levels become extremely elevated, often exceeding 600 mg/dL (33.3 mmol/L). HHS typically involves higher than average blood glucose levels compared to DKA.
- Relative Insulin Deficiency: Even though insulin may be present, its levels are insufficient to facilitate glucose uptake by cells and allow excess amounts of glucose into the bloodstream. This leads to an excess buildup of glucose which causes complications.
- Osmotic Diuresis: Elevated blood glucose levels cause osmotic diuresis, leading to excessive urination and fluid loss resulting in severe dehydration.
- Neurological Symptoms: HHS often manifests with neurological symptoms like confusion, altered consciousness, slurred speech, visual disturbances, weakness and seizures that are more pronounced compared to DKA. These signs and symptoms should also be looked out for when making decisions on whether DKA would be more appropriate as treatment option.
- Dehydration: Osmotic diuresis-caused dehydration contributes to dry skin, mouth dryness, sunken eyes and decreased skin turgor.
- Ketosis and Acidosis Are Absent: Unlike DKA, HHS doesn’t involve significant ketone production or metabolic acidosis resulting in less acidic blood conditions. The blood stays more alkaline.
- Lab Findings: Diagnostic criteria for HHS include blood glucose levels exceeding 600 mg/dL (33.3 mmol/L), increased serum osmolality and the absence of significant keton production and acidosis.
- Underlying Triggers: Infections, medications, stress and medical conditions can all play a part in HHS.
- Gradual Onset: HHS typically begins more gradually than DKA, allowing for prolonged exposure to elevated blood glucose levels before symptoms become severe.
HHS Has a Higher Mortality Rate Than DKA Due to its effects on the nervous system, increased risk for thromboembolic events, and complications caused by severe dehydration, HHS has an elevated mortality rate than DKA.
What are the causes of HHS?
Hyperosmolar Hyperglycemic State (HHS), often observed among those living with type 2 diabetes who are older or have impaired kidney function, results from several factors coming together at once; it involves both an insulin deficiency and increased resistance that contribute to this condition. Underlying medical conditions like infections, heart attacks, and kidney issues may contribute to insulin resistance and cause elevated blood glucose levels.
Medication changes that raise or alter glucose levels or alter insulin sensitivity could trigger HHS. Dehydration, typically found among older adults and those with impaired thirst perception, can occur from decreased fluid consumption or excessive loss due to infection or medications. Physical stressors such as surgery or trauma release stress hormones that counteract insulin and worsen hyperglycemia.
Non-adherence to diabetes medications, newly diagnosed cases with untreated high blood glucose, and advanced age can all increase HHS risks. Understanding these causes is key for preventing and managing HHS, such as by keeping glucose under control, increasing fluid intake, and seeking medical assistance promptly when illnesses or stresses arise.
Symptoms of HHS
Hyperosmolar Hyperglycemic State, more commonly known as hyperosmolar Hyperglycemic Nonketotic Syndrome (HHNS).
Usually develops gradually over time and its symptoms include:
- Extreme Thirst (Polydipsia): Individuals may experience extreme thirst and the persistent need to drink water.
- Frequent Urination (Polyuria): High blood glucose levels cause frequent urination as the urine output increases.
- Confusion and Altered Mental Status: High blood glucose levels affecting brain function often result in neurological symptoms like confusion, difficulty focusing, altered consciousness or altered mental status.
- Visual Disturbances: Blurred vision or changes in vision acuity may occur and require medical intervention to correct.
- Weakness and Fatigue: Poor glucose utilization by cells may result in weakness and fatigue across the board.
- Dehydration: Dehydration can result in dry skin and lips due to reduced water intake. Cracked Lips: Dehydration can cause cracked lips as well.
- Seizures and Coma: Untreated HHS may lead to seizures or coma due to its impact on the nervous system.
- Rapid Heart Rate and Low Blood Pressure: Dehydration and electrolyte imbalance can result in rapid heart rate and low blood pressure, both symptoms of dehydration.
- Hemiparesis: One side of your body may experience weakness due to neurological effects.
- Other Neurological Symptoms: Neurological symptoms can vary and could include hallucinations, tremors or focal neurological deficits.
Key Differences Between DKA and HHS
Here’s a comparison chart highlighting the key differences between Diabetic Ketoacidosis (DKA) and Hyperosmolar Hyperglycemic State (HHS):
| Aspect | Diabetic Ketoacidosis (DKA) | Hyperosmolar Hyperglycemic State (HHS) |
|---|---|---|
| Associated Diabetes Type | Primarily Type 1 diabetes | Primarily Type 2 diabetes |
| Insulin Deficiency | Severe | Relative |
| Ketosis and Acidosis | Present | Absent |
| Ketone Production | High | Low |
| Blood Glucose Levels | Typically >250 mg/dL (13.9 mmol/L) | Extremely elevated, often >600 mg/dL |
| pH Levels | Low (Acidic) | Normal to slightly low |
| Symptom Onset | Rapid | Gradual |
| Neurological Symptoms | Less prominent | More prominent |
| Fruity Breath Odor | Present | Absent |
| Fluid Loss | Dehydration due to osmotic diuresis | Severe dehydration |
| Electrolyte Imbalances | Common, particularly hypokalemia | Common, electrolyte imbalances |
| Confusion and Altered Mental | Less pronounced | More pronounced |
| Seizures and Coma Risk | Less common but possible | More common in severe cases |
| Serum Osmolality | Normal or slightly increased | Markedly increased |
| Typical Patient Profile | Younger with type 1 diabetes, rapid onset | Older with type 2 diabetes, gradual onset |
| Mortality Rate | Lower compared to HHS | Higher compared to DKA |
Diagnosed and Treatment
How is DKA and HHS diagnosed?
Diagnosing Diabetic Ketoacidosis (DKA) and Hyperosmolar Hyperglycemic State (HHS) requires a combination of clinical assessment, physical exam and laboratory tests. Key diagnostic criteria for each condition are as follows.
Diabetic Ketoacidosis (DKA):
- Blood Glucose Levels: Usually exceeding 250 mg/dL (13.9 mmol/L).
- Ketone Levels: An elevated presence of ketones in blood and urine.
- Artery pH Levels: Arterial blood pH lower than 7.3 indicates acidosis,
- Bicarbonate Levels: Bicarbonate Levels are below 18mEq/L which suggests low bicarbonate levels in the body.
- Anion Gap: Increased anion gap due to ketoacid accumulation.
- Clinical Presentation: Signs include excessive thirst, frequent urination, fruity breath odor, rapid breathing (Kussmaul breathing), and signs of dehydration.
Hyperosmolar Hyperglycemic State (HHS):
- Blood Glucose Levels: Extremely elevated glucose levels that often surpass 600 mg/dL (33.3 mmol/L).
- Serum Osmolality: Elevated due to hyperglycemia.
- Artery pH: Normal or slightly decreased with minimal or no acidosis present.
- Ketone Levels: An absence of ketosis both in blood and urine samples.
- Clinical Presentation: Neurological symptoms including confusion, altered consciousness, visual disturbances and severe dehydration can present themselves clinically.
DKA and HHS can both be diagnosed by conducting blood tests, such as measuring blood glucose, arterial blood gas analysis to measure pH and bicarbonate levels, and blood and urine ketone level assessments. Acidosis, ketosis (in DKA), and extreme hyperglycemia are key diagnostic features.
Clinical signs and symptoms such as dehydration and neurological changes help in making an accurate diagnosis; medical history review, physical exam evaluations, as well as sometimes additional testing to identify possible triggers (like infections or medication changes) all play an integral part in making an accurate diagnosis of these conditions.
Treatment of DKA and HHS
Diabetic Ketoacidosis (DKA) Treatment Options:
- Insulin Administration: Intravenous insulin is the cornerstone of treating DKA. It helps lower blood glucose levels while inhibiting the production of ketones. The infusion rate should be tailored based on blood glucose levels for gradual reduction.
- Fluid Replacement: Intravenous fluid replacement therapy is administered intravenously to address dehydration and maintain adequate circulation. At first, isotonic saline is used, gradually transitioning over to hypotonic fluids as blood glucose levels decrease.
- Electrolyte Management: Electrolyte imbalances, specifically potassium levels, must be carefully managed. While initial potassium levels may rise due to acidosis, their levels will likely fall once insulin therapy begins and decrease.
- Correcting Acidosis: Insulin therapy and fluid administration can assist in correcting metabolic acidosis by decreasing ketone production while simultaneously raising bicarbonate levels.
- Monitoring: Adequate monitoring of blood glucose, ketones, electrolytes and acid-base balance allows treatment providers to make adjustments quickly.
HHS (Hyperosmolar Hyperglycemic State) Treatment Options:
Fluid Replacement: Intravenous fluid replacement therapy using isotonic saline can quickly correct severe dehydration, helping avoid fluctuations in electrolyte levels that could otherwise result from sudden changes. Over time, gradual rehydration helps ensure proper electrolyte balance is restored.
Insulin Therapy: Insulin can be given intravenously to lower blood glucose levels. The rate of administration should be carefully adjusted to prevent rapid glucose reduction that could result in cerebral edema.
Electrolyte Correction: Any electrolyte imbalances, such as potassium abnormalities, are addressed as part of treatment.
Underlying Cause Identification: In order to address HHS episodes and avoid their recurrence, its triggers, such as infections or medications are identified and addressed to prevent future incidents.
Regular Monitoring: Conducting routine blood glucose, electrolyte, and overall clinical status monitoring helps guide treatment modifications.
Long-Term Effects of DKA and HHS on the Body
Experience of Diabetic Ketoacidosis (DKA) or Hyperosmolar Hyperglycemic State (HHS) can have lasting repercussions for individuals living with diabetes, even after its acute episodes have been treated.
Prolonged and severe hyperglycemia seen in both conditions may contribute to long-term complications in those living with the disease – creating acidic environments or extreme hyperglycemia can negatively impact organ systems throughout the body, with DKA producing acidity while HHS leads to hyperglycemia which impacts organ systems across systems alike.
Cardiovascular System: Both DKA and HHS can put a strain on the cardiovascular system. Consistent high blood glucose levels may damage blood vessels, increasing your risk for heart attacks, strokes, peripheral vascular disease, and more.
- Kidneys: Uncontrolled hyperglycemia associated with DKA and HHS has the potential to damage kidneys over time, potentially leading to diabetic nephropathy and chronic kidney disease.
- Nerve System: HHS may cause neurological symptoms, including confusion and altered consciousness, to indicate potential brain involvement. Over time, high blood glucose levels can lead to diabetic neuropathy, damaging nerves throughout the body and leading to symptoms like pain, numbness and impaired sensation in nerve endings throughout your body.
- Eyes: Diabetics at high glucose levels increase their risk for diabetic retinopathy, a condition in which damaged blood vessels in the eye damage vision and can even lead to blindness. If left unchecked, diabetes could result in vision problems or blindness.
- Gastrointestinal System: Nausea and vomiting associated with DKA can put undue strain on digestive health, while prolonged hyperglycemia may even contribute to gastroparesis – an illness in which stomach contents don’t empty correctly – over time.
- Immune System: Both conditions diminish an individual’s immune system’s capacity to fight infections effectively, with chronic hyperglycemia making individuals more prone to infections while delaying wound healing time.
- Metabolic Health: Repeated episodes of DKA and HHS can increase insulin resistance, further dismantling blood glucose control and contributing to overall metabolic dysfunction.
Complications and Prognosis of DKA and HHS
Diabetic Ketoacidosis (DKA) and Hyperosmolar Hyperglycemic State (HHS) are potentially life-threatening diabetic emergencies that should be promptly and effectively treated to avoid further complications. DKA may cause life-threatening cerebral edema (swelling of the brain), as well as electrolyte imbalances, hypokalemia and cardiac arrhythmias that require immediate medical attention.
DKA untreated can result in hypovolemic shock, acute kidney injury, acute respiratory distress syndrome (ARDS) or even death. HHS on the other hand increases your risk of thromboembolic events due to increased blood viscosity caused by extreme hyperglycemia.
HHS symptoms such as confusion, seizures and coma are highly alarming. Furthermore, dehydration associated with HHS may lead to hypovolemic shock, kidney damage and organ failure that require intensive medical attention for prevention purposes.
With timely treatment and management, the prognosis for both DKA and HHS can often be quite positive. A rapid intervention to restore fluid balance, manage electrolyte levels and lower blood glucose can quickly bring relief to symptoms while warding off further complications. However, the risk of complications does exist and its outcomes can depend on several factors including severity of initial presentation, overall health status, and presence of any underlying conditions.
Regular monitoring, adherence to treatment plans and follow-up care are vital in order to prevent recurrence of episodes as well as mitigate their long-term impact. Education on diabetes management including the identification of triggers and symptoms plays an invaluable role in mitigating risks associated with DKA/HHS emergencies.
How can you prevent DKA?
Preventing Diabetic Ketoacidosis (DKA) requires careful diabetes management and taking proactive measures to maintain stable blood glucose levels, among other strategies.
Here are several key strategies for avoiding DKA:
- Track Blood Glucose Levels Regularly: Checking your blood glucose levels as recommended by healthcare providers will allow you to catch and address high blood sugar levels before they worsen.
- Take Insulin Accordingly: Individuals living with type 1 or type 2 diabetes who require insulin should take it according to the instructions from their healthcare provider; failing to do so could result in insulin deficiency and lead to DKA. Missed doses could result in severe complications.
- Monitor Ketone Levels: For periods of illness and stress, urine or blood ketone testing should be used to track ketone levels. An increase in these may indicate an increased need for insulin doses.
- Maintain Hydration: Drink plenty of fluids throughout the day in order to avoid dehydration, an indicator of DKA. Adequate hydration helps maintain stable blood glucose levels.
- Manage Illness: While sick, your insulin requirements may increase significantly. Monitor your blood glucose regularly and continue taking your dose; seek medical guidance if necessary.
- Education: Be mindful of the early warning signs associated with DKA, such as excessive thirst, frequent urination and changes to breath odor. Learn the significance of seeking medical help immediately if symptoms arise.
- Regular Medical Appointments: Be sure to schedule regular appointments with your healthcare provider in order to evaluate how your diabetes management is progressing, make any necessary adjustments, and address any potential concerns.
- Insulin Pump Maintenance: When using an insulin pump, make sure it’s functioning as intended and dispensing insulin accurately.
- Stress Management: Take steps to effectively manage stress, as its hormones can raise blood glucose levels. Try engaging in stress-reducing methods like physical activity, meditation, or relaxation techniques such as yoga.
- Carb Counting: When counting carbohydrates to determine insulin doses, be consistent and accurate so as to prevent over- or underdosing.
- Medication Management: Individuals living with type 2 diabetes should administer oral medications and adapt lifestyle factors accordingly in order to avoid sudden spikes in their blood glucose levels.
- Travel Planning: Be prepared when traveling by bringing along sufficient insulin and supplies as well as having a plan in place to adjust to changes in time zones and routines.
- Communication: Stay in contact with your healthcare team, discussing any changes to your condition, medications or lifestyle that might alter how diabetes is managed.
summary
Diabetic Ketoacidosis (DKA) and Hyperosmolar Hyperglycemic State (HHS) are serious diabetes complications that must be managed quickly or else can have fatal consequences. DKA involves acidosis with subsequent ketone buildup; HHS involves severe hyperglycemia with subsequent dehydration.
Both conditions require immediate medical intervention; DKA can lead to cerebral edema and electrolyte imbalances while HHS poses an increased risk of thromboembolic events and neurological symptoms.
Treatment options for both conditions include insulin administration, fluid replacement and electrolyte correction; however early intervention and careful management can have beneficial outcomes Education regarding diabetes management will help to avoid and address such emergencies effectively.