Difference Between Streptokinase and tPA
Brief overview of Streptokinase and tPA
Streptokinase and tPA (tissue Plasminogen Activator) are two clot-dissolving medications widely used for treating certain medical conditions, respectively.
Here’s an introduction of each:
Streptokinase: Streptokinase, an naturally-derived enzyme from group C beta-hemolytic streptococci bacteria, works to activate plasminogen to form plasmin which then breaks down blood clots. For many years it has been used as an effective thrombolytic agent.
Streptokinase is often prescribed in cases of acute myocardial infarction (heart attack), deep vein thrombosis, and pulmonary embolism, as this enzyme helps dissolve any clots to restore blood flow to affected areas and restore health.
- Administration: Streptokinase should typically be given intravenously and the dosage and length of treatment depend upon which condition is being addressed.
- Potential Side Effects of Streptokinase: Possible adverse reactions may include bleeding, allergic reactions, low blood pressure, fever and flu-like symptoms.
TPA (Tissue Plasminogen Activator):
TPA, or tissue plasminogen activator, is an enzyme which activates plasminogen to produce plasmin that breaks down blood clots. Unlike streptokinase which uses chemicals as its activating source for making streptokinase active again by biotechnology methods, instead tPA uses synthetic biological proteins which have been produced using these biotech methods.
- Uses: TPA is most frequently employed for treating acute ischemic stroke, where it works to dissolve any blockages to blood flow to the brain. In addition, tPA may also help manage acute myocardial infarction or pulmonary embolism symptoms.
- Administration: tPA should be given intravenously and the exact dosage and administration protocols may differ for different conditions.
- Potential Side Effects of TPA: Some potential adverse reactions associated with taking TPA include brain bleeding as one major risk, allergic reactions, low blood pressure, or nausea could also arise as possible reactions.
Streptokinase and tPA both serve to dissolve blood clots, yet both come with their own set of advantages and drawbacks when used medicinally. Healthcare providers must carefully assess each patient to select an effective medication tailored specifically to his/her condition and characteristics to treat.
Importance of clot-dissolving therapy in medical emergencies
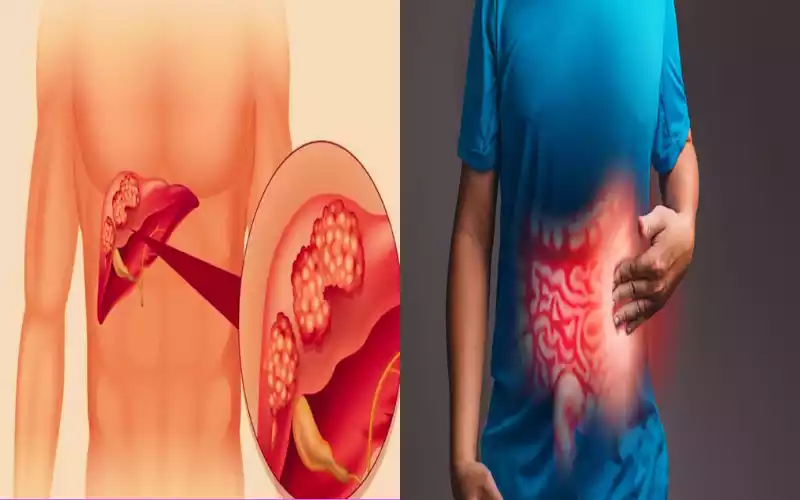
Clot-dissolving therapy cannot be understated as part of medical emergency responses. Clot formation, commonly referred to as thrombosis, can occur anywhere within the body and pose significant health risks. Clots can obstruct blood vessels allowing reduced or completely blocked circulation to vital organs leading to potentially life-threatening conditions including heart attacks, strokes and pulmonary embolism resulting in significant physical harm – potentially even heart attacks, strokes or even cardiac arrest in extreme instances.
Clot dissolving therapy (thrombolytic therapy) serves to break up and dissolve blood clots that obstruct circulation, thus restoring normal flow while also protecting against further damage to organs or systems.
Clot-dissolving therapies play an essential role in medical emergencies due to:
- An Ischemic Stroke: An ischemic stroke results when bloodflow to the brain is interrupted due to clotting, leading to tissue death in its wake. Administering clot-dissolving therapy quickly can restore blood flow, minimize brain damage and increase functional recovery rates.
- Acute Myocardial Infarction (Heart Attack): A heart attack occurs when a clot forms in one or more coronary arteries, blocking off blood supply to the heart muscle and restricting it further. Clot-dissolving therapy may quickly dissolve this obstruction to restore circulation while lessening muscle damage to restore blood flow quickly and reduce damage levels quickly, early administration will ensure maximum effectiveness from this approach.
- Pulmonary Embolism: Pulmonary embolism refers to any blockage of arterial branches by blood clots traveling from other parts of the body into the lungs, blocking arterial passageways. Clot-dissolving therapy may help dissolve these clots, improving lung function, alleviating symptoms and avoiding further complications.
- Deep Vein Thrombosis: Deep Venous Thrombosis (DVT) occurs when blood clots form in deep veins of either leg. Left untreated, they can dislodge and travel to the lungs resulting in pulmonary embolism, for severe cases of DVT clot-dissolving therapy may help quickly dissolve these clots to mitigate potential complications and lessen pain.
At times of medical urgency, timely administration of clot-dissolving therapy may save lives and improve patient outcomes significantly. It should be remembered, however, that not every individual may require this form of treatment and must carefully consider individual factors like location of clot formation as well as risks/benefits involved with each form of clot dissolution therapy before making their choice.
Healthcare professionals must recognize the signs and symptoms of medical emergencies quickly, initiate appropriate diagnostic evaluations as soon as they arise, and administer clot dissolving therapies immediately when indicated. Furthermore, ongoing research in this field seeks to enhance its efficacy and safety – further reinforcing its importance during medical emergencies.
Streptokinase
Streptokinase has long been used as an effective clot-dissolving medication and as a thrombolytic agent.
Here are a few important facts about streptokinase:
- Mechanism of Action: Streptokinase works by binding to and activating plasminogen, the precursor for the enzyme responsible for breaking down blood clots – plasmin. Once activated, this powerful anticoagulant degrades fibrin – the primary constituent of blood clots – leading to dissolution.
- Source and Production: Streptokinase is produced through fermentation processes using group C beta-hemolytic streptococci bacteria as the source. By cultivating these organisms in culture tanks, streptokinase production becomes an additional byproduct.
- Streptokinase is most frequently prescribed to treat acute myocardial infarction (heart attack), deep vein thrombosis (DVT), and pulmonary embolism (PE). By dissolving the blockages in blood flow, Streptokinase helps restore it quickly.
- Administration: Streptokinase should typically be administered intravenously under medical supervision in hospital settings. Dosage and duration will depend upon your specific condition being treated, so make sure the dosage and length of therapy fits for you!
- Potential Side Effects of Streptokinase: Some possible adverse reactions associated with Streptokinase include bleeding as the medication can break down blood clots throughout your body. Allergic reactions, low blood pressure, fever and flu-like symptoms could also occur as potential adverse reactions of this medicine.
- Contraindications and Precautions: Streptokinase should only be used with extreme caution in certain situations, including active bleeding, recent surgery/trauma, history of stroke or uncontrolled hypertension. Also it must not be administered when there is high risk of bleeding such as severe liver disease or compromised immunity system.
- Comparison to TPA: Streptokinase differs significantly from tissue plasminogen activator, or tPA, in its source, production method and potential side effects. TPA uses biotechnology methods while streptokinase comes directly from bacteria, as with many medical conditions being treated or risk/benefit assessments made individually, therefore their choice often hinges upon several variables including medical condition being addressed as well as patient specifics and individual risk-benefit considerations.
Healthcare professionals must carefully assess each patient’s current state, medical history and potential risks before prescribing streptokinase for use. Close monitoring must take place to prevent adverse side-effects while assuring optimal treatment outcomes.
Medical uses of Streptokinase
Streptokinase is widely utilized as an effective thrombolytic agent to treat various medical conditions.
Some examples include:
- Acute Myocardial Infarction (AMI): Streptokinase can help treat acute myocardial infarction (AMI), commonly referred to as a heart attack. By dissolving blood clots obstructing coronary arteries and restoring circulation to heart muscle, Streptokinase facilitates recovery from AMI.
- Deep Vein Thrombosis (DVT): Streptokinase can help treat deep vein thrombosis (DVT), where blood clots form in deep veins of legs. By dissolving and restoring normal blood flow to affected regions, Streptokinase reduces complications like pulmonary embolism while improving quality of life for sufferers.
- Pulmonary Embolism (PE): Streptokinase may help treat pulmonary embolism (PE), in which a blood clot blocks one or more vessels in the lungs and prevents normal blood flow to these vital organs and oxygenation levels from increasing as a result of decreased oxygen saturation levels in blood vessel walls. Dissolving blood clots by dissolving them with streptokinase helps restore proper oxygenation levels to these critical areas and allows proper oxygen exchange with them, improving oxygenation as a result.
- Arterial Thrombosis: Streptokinase has proven useful in treating arterial thrombosis, where blood clots form in arteries leading to reduced circulation to vital organs, by dissolving them quickly and returning normal flow of blood into them. By dissolving them quickly and returning normal flow again.
Notably, streptokinase’s efficacy may vary based on factors like clinical presentation, extent of clot burden and treatment guidelines outlined for individuals. Healthcare professionals usually determine dosage based on both patient condition being addressed as well as characteristics unique to that patient.
tPA (Tissue Plasminogen Activator)
tPA (Tissue Plasminogen Activator) is an anticoagulant medication prescribed to treat certain medical conditions, specifically blood clots.
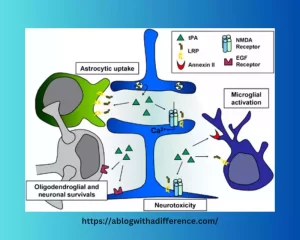
Here are a few key points about its usage:
- Mechanism of Action: tPA is an enzyme produced naturally within our bodies that plays an integral part in breaking down blood clots. When administered as medication, tPA binds with fibrin components of blood clots and converts plasminogen to plasmin. eventually leading to its dissolution and the dissolving of fibrin meshes within blood clots.
- Production: Therapeutic Grade TPA (tPA) used in medical treatments is manufactured using recombinant DNA technology. To produce large-scale quantities, its gene must be introduced into host cells such as bacteria or mammalian cells which then produce it rapidly and mass produce it.
- Indications for Use: tPA is often prescribed to treat acute ischemic stroke, in which blood clots block an artery leading directly into the brain. Additionally, it has proven successful at managing myocardial infarction (heart attack) and pulmonary embolism (PE), in which blood clots impede circulation to either heart or lungs respectively.
- Administration: Treatment with tPA typically involves intravenous administration. dosage, infusion rate and duration will depend upon both the condition being addressed as well as individual circumstances. It’s best to start therapy immediately following symptoms’ onset for optimal effectiveness.
- Potential Side Effects: Administration of tPA can pose the risk of bleeding complications as the medication works to break up blood clots within the body. Bleeding within the brain, with potentially life-threatening repercussions, is likely the most alarming side effect. other possible reactions include allergic reactions, low blood pressure, nausea and vomiting.
- Contraindications and Precautions of TPA Therapy: TPA should not be administered when active bleeding, recent surgery, history of stroke or head injury, uncontrolled hypertension or bleeding disorders exist. additional precaution should be exercised with patients at increased risk for bleeding such as those recently traumatized or suffering from certain medical conditions.
- Comparison to Streptokinase: TPA differs significantly from streptokinase when it comes to its production, potential side effects and indications. Streptokinase comes from bacteria while TPA uses biotechnology methods. which one you use ultimately depends upon factors like medical condition being treated, patient characteristics and risk assessment.
Healthcare professionals must carefully assess a patient’s eligibility for tPA therapy, considering both timing of therapy initiation as well as potential risks and benefits. Close monitoring and management of complications during and post administration to maximize treatment results while protecting patient safety and ensure safe care delivery.
Medical uses of tPA (tissue Plasminogen Activator)
TPA (Tissue Plasminogen Activator) is an anticoagulant medication commonly prescribed to treat various medical conditions; specifically:
- Acute Ischemic Stroke: tPA can be effective against acute ischemic stroke, which occurs when blood clots block an artery feeding the brain, by dissolving them quickly after symptoms arise and restoring blood flow back to affected regions, potentially decreasing disability and improving outcomes. Administering it within certain time windows after symptoms have begun may help dissolve any blockages, disperse blood clots and restore flow; potentially decreasing disability while improving outcomes and outcomes for treatment of acute stroke patients.
- Acute Myocardial Infarction (AMI): tPA may be effective against acute myocardial infarction (also referred to as heart attacks). It works by dissolving blood clots that block coronary arteries, providing adequate blood flow back into heart muscle and thus decreasing damage.
- Pulmonary Embolism (PE): tPA can help manage pulmonary embolism (PE), in which a blood clot blocks one or more vessels in the lungs and restricts their blood flow and oxygenation of lung tissue. By administering this drug, however, this blockage may be dissipated so blood flow and oxygenation of lung tissue improve.
As it should be noted, using tPA for certain medical conditions requires immediate action and has specific eligibility and treatment guidelines. Care must be taken by healthcare providers when administering this therapy to ensure patient safety while simultaneously reaping maximum potential clot dissolving benefits. Dosage, infusion rate and duration vary based on both medical condition being treated and individual patient characteristics.
Differences Between Streptokinase and tPA
The differences between Streptokinase and tPA (Tissue Plasminogen Activator) can be summarized in the following points:
- Source and Production:
- Streptokinase: It is derived from group C beta-hemolytic streptococci bacteria through fermentation processes.
- tPA: It is produced using recombinant DNA technology, where the gene responsible for producing tPA is inserted into host cells for large-scale production.
- Mechanism of Action:
- Streptokinase: It binds to and activates plasminogen, which leads to the conversion of plasminogen into plasmin. Plasmin breaks down fibrin, the main component of blood clots.
- tPA: It directly activates plasminogen to plasmin, initiating the breakdown of fibrin and subsequent clot dissolution.
- Indications:
- Streptokinase: It is primarily used in the treatment of acute myocardial infarction (heart attack), deep vein thrombosis (DVT), and pulmonary embolism (PE).
- tPA: It is commonly used in the treatment of acute ischemic stroke, acute myocardial infarction, and pulmonary embolism.
- Administration and Dosage:
- Streptokinase: It is typically administered intravenously. The dosage and treatment duration vary depending on the specific condition being treated.
- tPA: It is also administered intravenously, and the dosage and infusion rate depend on the specific indication and patient characteristics.
- Side Effects and Complications:
- Streptokinase: Potential side effects include bleeding, allergic reactions, low blood pressure, fever, and flu-like symptoms.
- tPA: The main concern with tPA is the risk of bleeding, especially in the brain, which can lead to serious complications. Other possible side effects include allergic reactions, low blood pressure, and nausea.
- Contraindications and Precautions:
- Streptokinase: It is contraindicated in active bleeding, recent surgery or trauma, history of stroke, uncontrolled hypertension, and certain other conditions. Precautions should be taken in patients with a high risk of bleeding or compromised immune system.
- tPA: It is contraindicated in active bleeding, recent major surgery or trauma, history of stroke or intracranial hemorrhage, uncontrolled hypertension, and other specific conditions. Precautions should be taken in patients with an increased risk of bleeding or certain medical conditions.
The choice between Streptokinase and tPA depends on various factors, including the specific medical condition being treated, patient characteristics, risk assessment, and availability. Healthcare professionals evaluate these factors to determine the most appropriate clot-dissolving medication for each individual case.
Comparison chart
Here’s a comparison chart differences between Streptokinase and tPA:
| Aspect | Streptokinase | tPA (Tissue Plasminogen Activator) |
|---|---|---|
| Source | Derived from group C beta-hemolytic streptococci bacteria | Produced using recombinant DNA technology |
| Mechanism of Action | Activates plasminogen to plasmin | Directly activates plasminogen to plasmin |
| Indications | Acute myocardial infarction, DVT, PE | Acute ischemic stroke, AMI, PE |
| Administration | Intravenous | Intravenous |
| Potential Side Effects | Bleeding, allergic reactions, low blood pressure | Bleeding (including intracranial), allergic reactions |
| Contraindications | Active bleeding, recent surgery/trauma, history of stroke, uncontrolled hypertension | Active bleeding, recent surgery/trauma, history of stroke/intracranial hemorrhage, uncontrolled hypertension |
| Production | Derived from bacteria through fermentation processes | Produced using recombinant DNA technology |
Similarities Between Streptokinase and tPA
Streptokinase and TPA (Tissue Plasminogen Activator) may share similarities when used to dissolve blood clots.
Here are their key similarities:
- Mechanism of Action: Streptokinase and tPA work by activating plasminogen to activate plasmin, leading to its conversion into the enzyme responsible for breaking down fibrin–one of the primary components of blood clots–thereby dissolving them and improving circulation. Both medications ultimately aim to promote dissolution while improving flow restoration.
- Thrombolytic Agents: Streptokinase and tPA are classified as thrombolytic agents. Used in emergency settings where fast dissolution of blood clots is essential to patient outcomes such as acute myocardial infarction, deep vein thrombosis, pulmonary embolism or acute ischemic stroke, these agents help ensure successful patient recovery.
- Intravenous Administration: Both medications should typically be given intravenously for maximum rapidity in distribution and action across your entire body. They will enter directly into the bloodstream.
- Potential Side Effects: Both Streptokinase and tPA may increase bleeding tendencies as a possible side effect of their use. due to dissolving blood clots and increasing bleeding tendencies during their administration, proper monitoring must take place as well as consideration for risks or contraindications for safe administration of both medications.
- Considerations in Treatment: Streptokinase and tPA need to be prescribed according to each individual patient’s unique medical history, condition and risk factors. Then selected according to indication, timing and suitability for use in each instance.
Though these medications share similarities, there are distinct differences that need to be considered when making decisions between Streptokinase and tPA for dissolving blood clots in different patients. Therefore, healthcare providers carefully assess each case when prescribing appropriate clot-dissolving medicine to their respective patient conditions.
Conclusion
Streptokinase and tPA (tissue Plasminogen Activator) are two clot-dissolving medicines commonly prescribed to treat various medical conditions, with Streptokinase being produced using bacteria while TPA uses recombinant DNA technology. both medications work by activating plasminogen while Streptokinase directly activates it. they differ significantly in terms of how they’re take. Streptokinase may activate it via activating it whilst TPA works differently by directly activating its activating its activating it directly. Streptokinase may activate it while TPA may directly activate it directly plasminogen directly, making both medications ideal in terms of usage. Streptokinase can treat acute myocardial infarction, deep vein thrombosis or pulmonary embolism while TPA may treat acute ischemic stroke, acute myocardial infarction as well.